Nursing education undergoes a dramatic move as technology reshapes how students master clinical skills. Traditional methods of teaching hands-on competencies are being boosted, and innovative digital solutions sometimes replace them to bridge the gap between theory and practice.
Nursing education requirements become more rigorous and clinical placements harder to secure. Forward-thinking companies step up to provide expandable, effective alternatives. We’ll explore four companies leading this transformation in this piece, each offering unique approaches to preparing the next generation of nurses for real-life patient care.
Nursa

Clinical placement coordination has long been one of the most complex administrative challenges in nursing education. Nursing programs often find themselves buried in paperwork rather than focused on student outcomes as they track compliance requirements, manage facility relationships, and schedule hundreds of students at multiple sites of all types. Nursa Study emerged as a direct response to this operational bottleneck, offering a purpose-built approach to clinical placement management that helps schools centralize and streamline these processes.
Nursa Study stands apart because of its foundation within a larger healthcare workforce ecosystem. The platform is part of the Nursa family of healthcare workforce solutions, which extends the company’s mission to support nurses and institutions powering patient care. This connection matters because it gives the clinical placement platform access to an existing network of healthcare facilities and nursing professionals that the parent company has built since its founding in 2019.
The broader Nursa marketplace operates as a nationwide staffing platform connecting healthcare facilities with qualified clinicians for per diem shifts. Facilities post open shifts in real-time. Nurses can browse and select assignments that fit their schedules. This flexibility has proven effective. Facilities using Nursa fill three times as many open per diem shifts compared to filling them independently. The Joint Commission recognized this operational success by awarding Nursa the Gold Seal of Approval certification for maintaining high standards of qualified and competent services. The company’s performance earned it recognition as a Utah Top Workplace for 2025.
Nursa’s offering creates a unique value proposition for nursing education through its dual nature. Programs gain administrative efficiency through Nursa Study’s placement management tools while connecting their students to a verified network of healthcare facilities that already use the broader Nursa staffing marketplace.
DaVinci Education
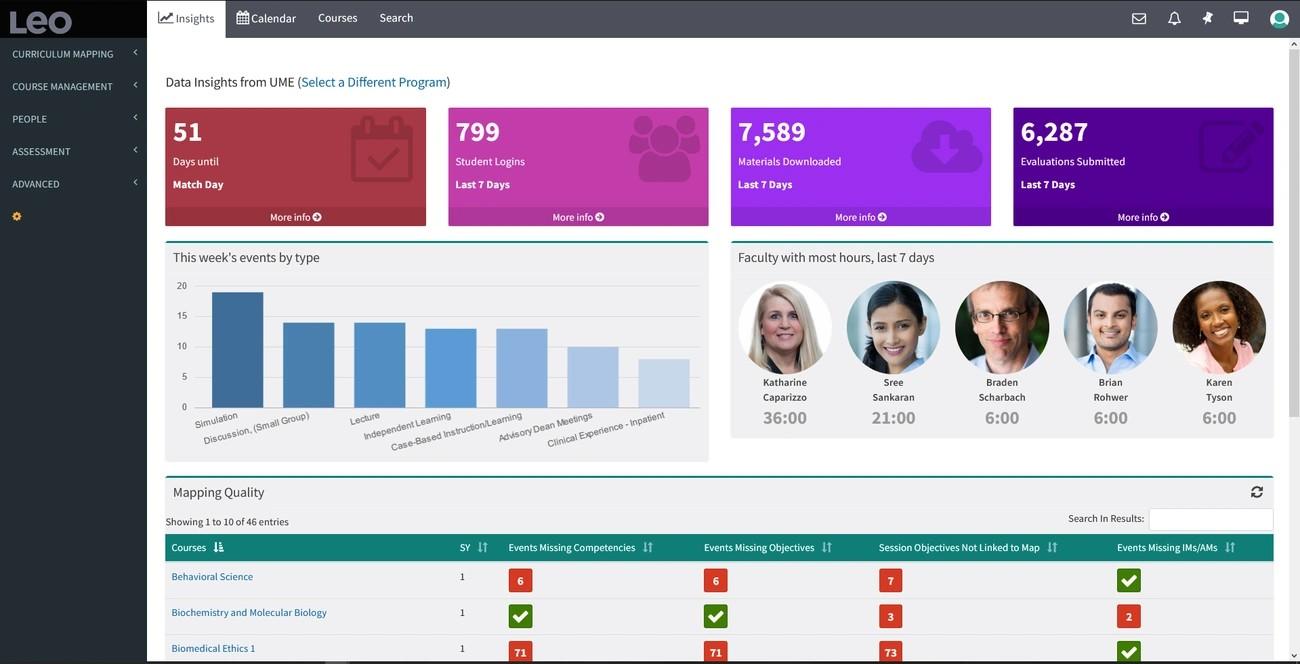
Enterprise software architecture can make or break a health sciences program’s operational efficiency. DaVinci Education recognized this reality when it developed Leo, an integrated platform built to unite the fragmented technology landscape that nursing education programs and other health sciences disciplines guide daily.
The platform emerged from a collaborative effort at Duke University School of Medicine more than a decade ago. Forward-looking administrators and educators at Duke identified a critical problem: programs were using too many disconnected systems to manage too many functions. This fragmentation created inefficiencies that rippled through every aspect of program administration. DaVinci Education responded by creating Leo as a unified solution designed to address these operational bottlenecks.
Clinical assessment represents where Leo distinguishes itself most. Nursing programs face a logistical puzzle: they need multiple off-site evaluators to complete student evaluations throughout the curriculum. Coordinating these assessments across distributed clinical sites required extensive administrative overhead. Leo simplifies this process through an approach that uses everyone’s most familiar technology tool: email.
Leo delivers insights on student performance, faculty effectiveness, and overall program outcomes that can improve results across the institution. These insights emerge from the unified data structure that integration enables. When all teaching, learning, assessment, and administrative functions operate within a single platform, programs can analyze relationships and patterns that remain invisible when data sits in isolated systems.
Elentra
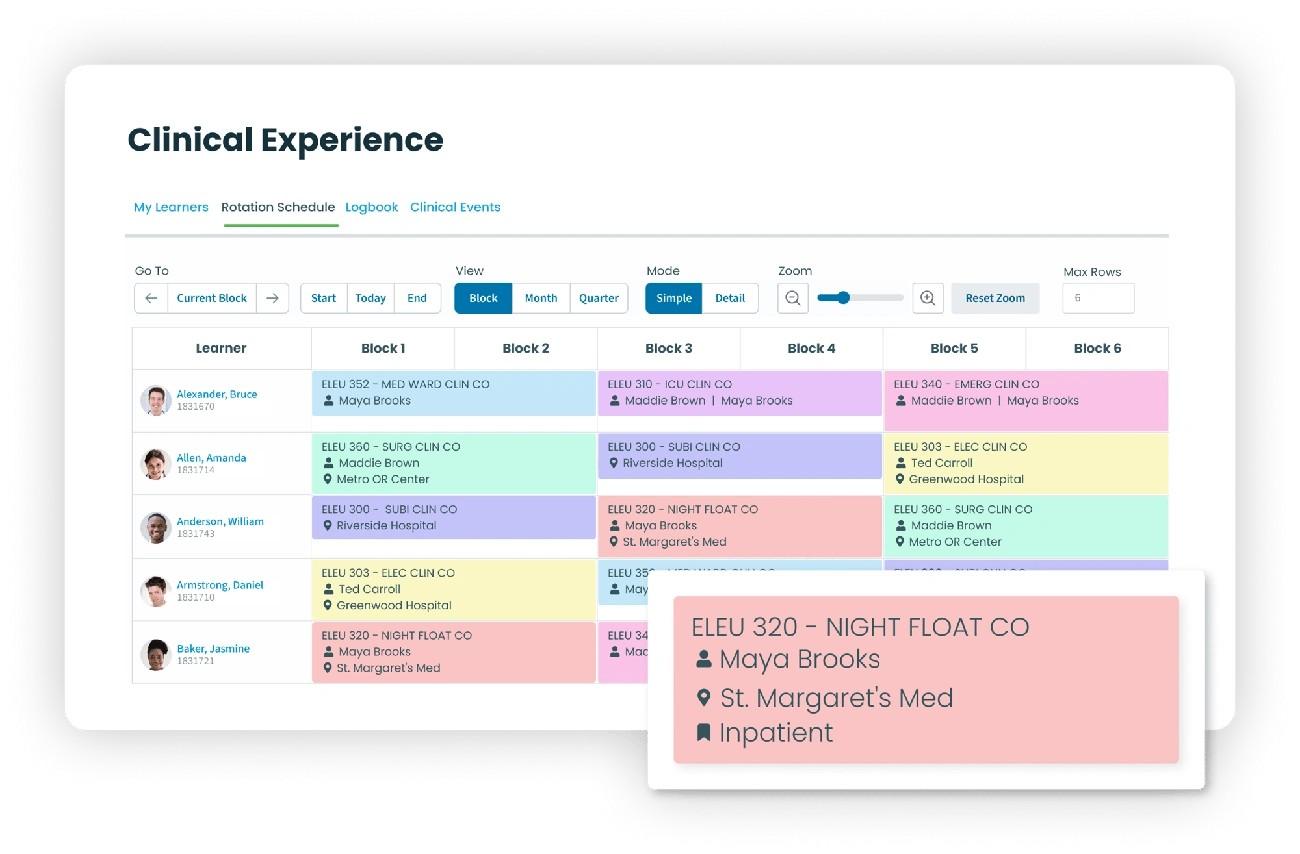
Collaborative development models in educational technology often promise institutional input but rarely deliver genuine co-governance. Elentra took a different path from its inception and built a platform through actual partnership rather than vendor-client relationships. Founded in 2008, Elentra emerged from collaboration between Queen’s University, the University of Calgary, and UCLA. These three institutions shared a common frustration: managing increasingly complex health sciences curricula while supporting faculty, learners, and accreditation coverage with tools that weren’t designed for healthcare education’s unique demands.
The solution they created became known as Elentra, an open-source system grounded in availability, extensibility, and academic stewardship. Unlike typical software companies that build products and sell them to schools, Elentra operated through a consortium model where member institutions co-developed and co-governed the platform. This structure proved functional rather than ornamental. Faculty and administrators gained direct influence over the tools they used daily. Every boost emerged from real institutional needs rather than vendor assumptions about what schools required.
Clinical rotation scheduling represents where Elentra separates itself through sophisticated automation. The platform streamlines the process of organizing and managing clinical rotations across healthcare facilities of all types. Clinical coordinators can schedule and manage students’ placements without drowning in spreadsheets or email coordination.
Competency mapping for nursing programs addresses accreditation’s most demanding requirements. Elentra supports mapping nursing competencies such as pharmacology, health assessment, and patient safety to standards from multiple accrediting bodies: the Commission on Collegiate Nursing Education (CCNE), the Accreditation Commission for Education in Nursing (ACEN), NLN Commission for Nursing Education Accreditation (CNEA), and the Canadian Association of Schools of Nursing (CASN). Programs can monitor progression, ensure curriculum alignment, and maintain accreditation readiness.
Shadow Health
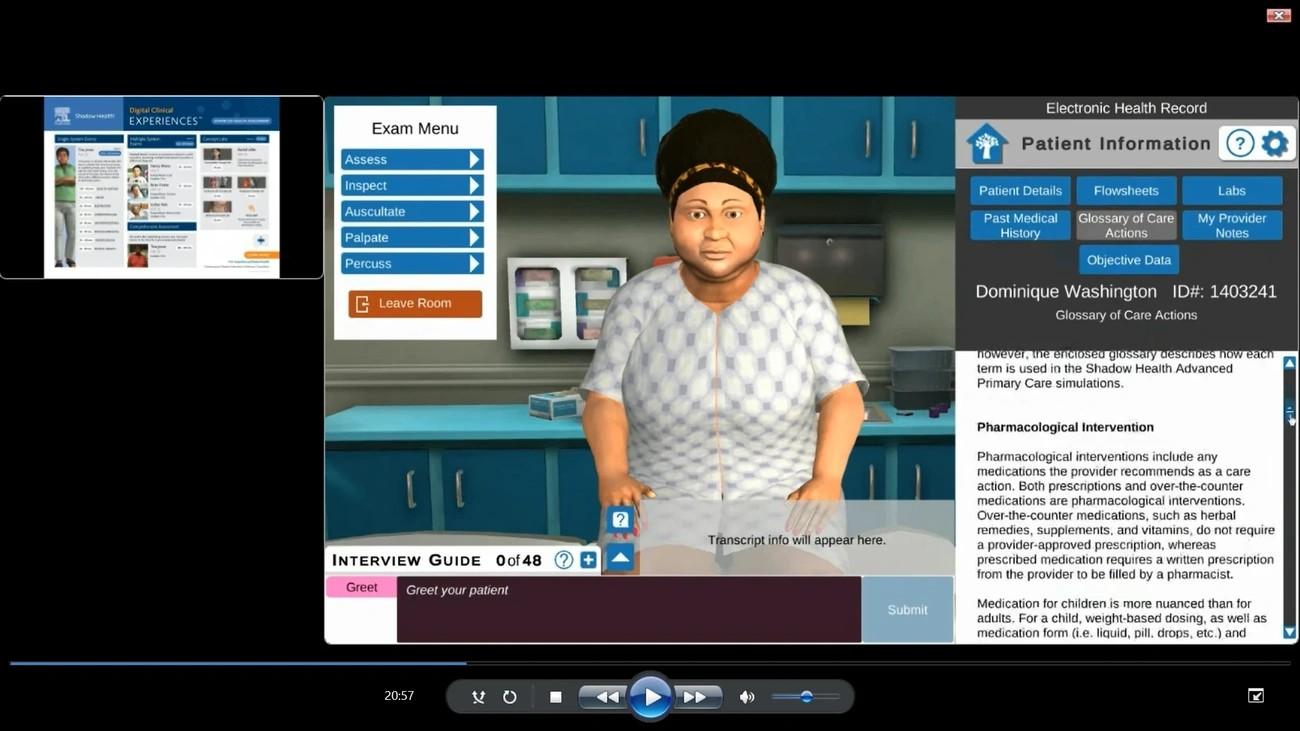
Virtual patient interactions represent the frontier where nursing education requirements meet clinical reality. Shadow Health, founded in Gainesville, Florida in 2011, built its platform around a single premise: students need to practice patient communication and clinical reasoning in environments that respond authentically to their choices without putting real patients at risk.
The company’s Digital Clinical Experiences deploy Digital Standardized Patients across scenarios spanning Fundamentals to Advanced Primary Care. What separates these simulations from scripted alternatives is the patented Conversation Engine that allows students to use their own words rather than selecting from predetermined dialog options. This technology makes 80+ diverse patients answer millions of unique questions and creates interactions that mirror the unpredictability of actual clinical encounters.
More than 700,000 nursing students have used Shadow Health to practice essential skills including patient interviews, physical exams, EHR documentation, and therapeutic communication. The platform serves both undergraduate students developing clinical reasoning skills and graduate students refining diagnostic reasoning capabilities. Content arranges with AACN Essentials competencies and ensures that simulation experiences map directly to nursing education requirements programs must meet for accreditation.
The feedback mechanisms embedded in each Digital Clinical Experience provide students with detailed performance data. Students compare their approaches against expert notes following virtual patient examinations and receive specific assessments of their clinical reasoning and practice readiness. Dynamic scenarios adapt based on student decisions and build clinical judgment skills through consequences rather than lectures.
Conclusion
Nursing education is entering a new phase as technology reshapes how students develop clinical skills. Traditional approaches to hands-on training still play an essential role, yet digital tools now enhance learning and help connect classroom knowledge with real patient care. These innovations support stronger preparation and give students more opportunities to build confidence before stepping into clinical environments.
At the same time, program requirements continue to grow more demanding while clinical placements become harder to secure. In response, forward-thinking companies are creating scalable solutions that support both educators and students. This article highlights four organizations helping to redefine clinical training in 2026, each offering a distinct approach to preparing future nurses for the realities of modern healthcare.






